Top Hospitals for Urology Surgery View All 
Best Doctors for Urology Surgery View All 
Senior Consultant - Urology
CONSULTS AT EXPEREIENCE :38 years SURGERIES :
NA
Treatment Price on request
Free Text ConsultTreatment Price on request
38 years SURGERIES :
NA TREATMENT COST
Treatment Price on request
Treatment Price on request
Free Text ConsultTreatment Price on request
5 years SURGERIES :
1000+ TREATMENT COST
Treatment Price on request
Urology Surgery
CONSULTS ATKrabi Nakharin International Hospital
EXPEREIENCE :NA years SURGERIES :
NA
Treatment Price on request
Free Text ConsultTreatment Price on request
NA years SURGERIES :
NA TREATMENT COST
Treatment Price on request
Senior Consultant - Pediatric Surgery & Pediatric Urology
CONSULTS ATBLK-Max Super Speciality Hospital, New Delhi
EXPEREIENCE :17+ years SURGERIES :
NA
Treatment Price on request
Free Text ConsultTreatment Price on request
17+ years SURGERIES :
NA TREATMENT COST
Treatment Price on request
Urology (genito-urinary)
CONSULTS ATBumrungrad International Hospital
EXPEREIENCE :18 years SURGERIES :
NA
Treatment Price on request
Free Text ConsultTreatment Price on request
18 years SURGERIES :
NA TREATMENT COST
Treatment Price on request
Treatment Price on request
Free Text ConsultTreatment Price on request
7 years SURGERIES :
NA TREATMENT COST
Treatment Price on request
Testimonials
View All 
Related Blogs
View All 

Erectile Dysfunction Treatment Cost in India
IntroductionErectile dysfunction (ED) is a prevalent condition that affects men of all ages worldwide. It can lead to significant emotional distress and strained relationships. Fortunately, there are various treatment options available, and India has emerged as a destination where individuals can access high-quality ED treatments at a fraction of the cost compared to many Western countries. In this blog, we will explore the various treatment options for ED in India and their associated costs.Understanding Erectile DysfunctionBefore delving into the costs of treating ED in India, it's essential to have a basic understanding of the condition. ED, often referred to as impotence, is the inability to achieve or sustain an erection sufficient for sexual activity. It can be caused by physical, psychological, or a combination of factors. Common causes include diabetes, cardiovascular diseases, stress, anxiety, and relationship issues.Treatment Options for Erectile DysfunctionLifestyle Changes: The initial step in treating ED often involves making lifestyle changes. These changes may include adopting a healthier diet, regular exercise, smoking cessation, and limiting alcohol consumption.Medications: Oral medications like sildenafil (Viagra), tadalafil (Cialis), and vardenafil (Levitra) are commonly prescribed to treat ED. These drugs work by enhancing blood flow to the penis, facilitating erections when sexually stimulated.Vacuum Devices: Vacuum erection devices (VEDs) are non-invasive devices that create a vacuum around the penis, drawing blood into it and facilitating an erection.Penile Injections: Intracavernosal injections of medications like alprostadil can be used to induce erections. This method is highly effective but requires a prescription and proper training for self-administration.Penile Implants: Surgical options, such as penile implants, are available for individuals who do not respond to other treatments. Penile implants involve surgically placing a device within the penis to simulate an erection when desired.Cost of Erectile Dysfunction Treatment in IndiaOne of the primary reasons why many people from around the world choose to seek ED treatment in India is the significantly lower cost of medical procedures and medications. Here's a breakdown of the approximate costs for different ED treatments in India:Oral Medications: A month's supply of popular ED medications like sildenafil or tadalafil can cost between $20 to $40 USD, depending on the brand and dosage.Vacuum Devices: High-quality vacuum erection devices are available for around $40 to $70 USD.Penile Injections: The cost of a single injection of alprostadil can range from $20 to $40 USD. A prescription from a urologist is required.Penile Implants: The cost of penile implant surgery in India varies depending on the type of implant chosen and the hospital or clinic. On average, it can range from $2,000 to $4,000 USD, including surgeon fees, hospital charges, and post-operative care.ConclusionErectile dysfunction is a common condition that can have a profound impact on a man's quality of life and relationships. Fortunately, there are various effective treatments available, and India has become a sought-after destination for ED treatment due to its affordability without compromising on quality.Before opting for any treatment, it's crucial to consult with a qualified urologist or sexual health specialist to determine the most suitable approach for your specific situation. Additionally, remember that the cost of treatment may vary based on factors such as the city, healthcare facility, and individual needs. Overall, seeking treatment for ED in India can provide cost-effective solutions, allowing individuals to regain their sexual confidence and improve their overall well-being.

Comprehensive Guide to Urethral Stricture Surgery in India: Top Doctors, Costs & Procedures
Introduction: Urethral stricture is a medical condition that affects the urinary system, causing narrowing or blockage of the urethra, the tube through which urine flows out of the body. This condition can lead to various urinary problems and discomfort. Fortunately, India offers world-class medical facilities and highly skilled urologists who specialize in urethral stricture surgery. In this comprehensive guide, we will explore the top doctors, costs, and procedures for urethral stricture surgery in India.Understanding Urethral Stricture: A urethral stricture occurs when scar tissue, inflammation, or other factors cause the urethra to become narrow or blocked. Common symptoms include difficulty urinating, weak urine flow, frequent urination, and urinary tract infections. If left untreated, urethral strictures can lead to more severe complications, making timely diagnosis and treatment essential.Urethral Stricture Surgery Procedures:Urethrotomy: This minimally invasive procedure involves the use of a laser or endoscope to incise the stricture, widening the urethral passage. Urethrotomy is often performed on an outpatient basis and has a relatively short recovery time.Urethroplasty: Urethroplasty is a more complex surgical procedure that involves removing the scar tissue and reconstructing the urethra. It is highly effective for long-term relief and is typically recommended for more severe strictures.Dilation: Urethral dilation is a non-surgical option that involves gently stretching the narrowed urethra using progressively larger tubes or dilators. While it can provide temporary relief, the stricture may recur.Top Urologists Specializing in Urethral Stricture Surgery in India:Dr. Ashutosh BaghelNephrologist / Urologist at : Wockhardt Hospitals, Mira Road, MumbaiDr. Ashutosh Baghel is a Urologist at Wockhardt Hospital, Mira Road, Mumbai, with 16 years of experience in Urology.His expertise covers various areas, including Onco-Urology, Stone Diseases (Kidney, Ureter, Bladder), Laser Surgery, Infertility, Arterio Venous Fistula (AVF), Renal Transplant, and Laparoscopic & Robotic Urology. Dr. Pramod. S. Consultant - Urologist at : Kauvery Hospital, ChennaiDr. Pramod S. is a well-tainted urologist based in Bengaluru, with over 7 years of experience.He is an expert in urinary stone disease, laser prostatectomy, andrology, and male sexual dysfunction. Cost of Urethral Stricture Surgery in India: The cost of urethral stricture surgery in India can vary depending on the procedure, the surgeon's experience, and the hospital's location. On average, urethrotomy may cost between $1,500 to $3,000, while urethroplasty may range from $3,000 to $6,000. Dilation procedures are generally more affordable, with costs ranging from $500 to $1,500.Preparing for Urethral Stricture Surgery:Consult with a urologist to determine the most suitable procedure for your condition.Share your medical history, including any allergies or medications you are taking.Follow pre-operative instructions provided by your surgeon, such as fasting before the surgery.Recovery and Aftercare: Recovery times vary depending on the procedure, but patients are typically advised to:Rest and avoid strenuous activities.Stay hydrated and follow a recommended diet.Take prescribed medications as directed.Attend follow-up appointments for monitoring.Conclusion:Urethral stricture surgery in India is a viable option for individuals seeking effective treatment from highly skilled urologists at a fraction of the cost compared to many Western countries. By choosing the right procedure and consulting with experienced doctors, patients can regain their quality of life and enjoy relief from urethral strictures.
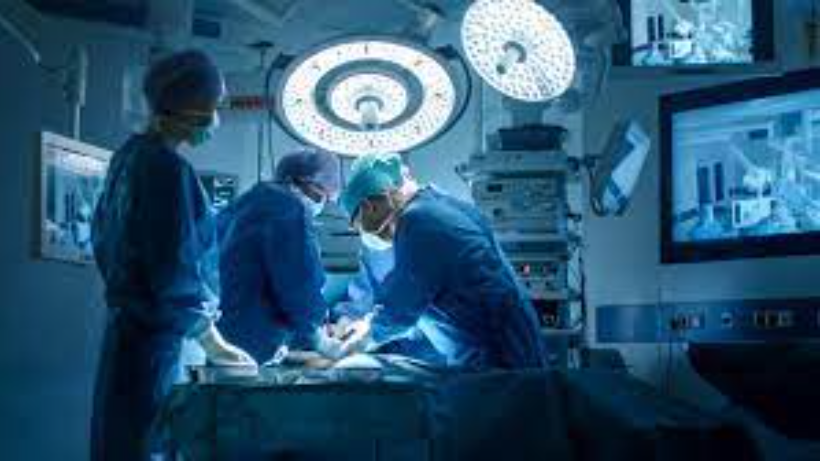
Understanding the Depths: A Comprehensive Guide to Pelvic Surgery
Pelvic surgery—a journey marked by challenges, resilience, and transformation. In this concise guide, we invite you to unravel the mysteries behind pelvic surgeries, understanding the reasons behind them and discover the individuals who may find solace in these procedures. From the careful preparations before surgery to the nuances of recovery, join us in shedding light on the intricacies of pelvic surgery.What is Pelvic surgery?Pelvic surgery is a medical procedure that deals with surgeries in the pelvic region, focusing on organs like the reproductive organs, bladder, and rectum. It's a broad category encompassing various surgical interventions to address conditions affecting these crucial parts of our body. These conditions can range from issues related to reproductive health, such as fibroids or endometriosis, to dealing with problems like pelvic organ prolapse. Essentially, pelvic surgery is a specialized field aiming to restore and improve the health and function of organs within the pelvic area.Purpose and Recipients of Pelvic SurgeryPelvic surgery serves distinct purposes, addressing a range of health issues affecting the pelvic region. Additionally, it is tailored to specific groups of individuals based on their health conditions.A. Why Pelvic Surgery is Done1. Treatment of Gynecological Conditions:Pelvic surgery is often employed to address various gynecological issues affecting women.Conditions like fibroids and endometriosis, which can cause pain, abnormal bleeding, and reproductive health challenges, may require surgical intervention.2. Management of Urological Disorders:Pelvic surgery plays a crucial role in managing disorders related to the urinary system.Individuals experiencing urinary incontinence or other urological issues may undergo pelvic surgery to restore normal function and alleviate associated symptoms.3. Correction of Pelvic Organ Prolapse:Pelvic organ prolapse occurs when pelvic organs such as the uterus, bladder, or rectum shift from their normal positions.Pelvic surgery is employed to reposition and provide support to these organs, addressing discomfort and potential complications associated with prolapse.B. Who Needs Pelvic SurgeryWomen are more likely than men to have pelvic surgery. This is because women have more organs in the pelvis.1. Women with Gynecological Issues (e.g., fibroids, endometriosis):Women experiencing conditions affecting the female reproductive system may require pelvic surgery for effective treatment.Fibroids, which are non-cancerous growths in the uterus, or endometriosis, a condition where tissue similar to the lining of the uterus grows outside the uterus.2. Individuals with Urological Disorders (e.g., urinary incontinence):Pelvic surgery is a viable option for those facing challenges related to urinary function.Surgical procedures can be recommended for individuals dealing with urinary incontinence, a condition characterized by the involuntary leakage of urine.3. Patients with Pelvic Organ Prolapse:Pelvic organ prolapse requires surgical correction to restore proper positioning and function of the affected organs.Women experiencing symptoms such as pelvic pressure, discomfort, or difficulty with bowel movements due to prolapse may benefit from pelvic surgery.Pelvic Surgery ProcedureA. Before the SurgeryPreoperative Evaluation:Before undergoing pelvic surgery, a comprehensive assessment is conducted to evaluate the patient's overall health.This evaluation helps identify any pre-existing conditions, assesses potential risks, and ensures the patient is physically prepared for surgery.Patient Counseling and Informed Consent:Patients receive detailed information about the upcoming surgery, including potential risks, benefits, and alternatives.It involves obtaining the patient's explicit agreement to undergo the procedure after understanding the relevant details.Preparing for Anesthesia:Patients meet with an anesthesia provider to discuss the type of anesthesia to be used and address any concerns.Specific guidelines, such as fasting before surgery, are provided to prepare the patient for anesthesia administration.B. During the SurgeryTypes of Pelvic Surgery (e.g., hysterectomy, bladder suspension):Removal of the uterus, often performed for conditions like cancer, fibroids, or severe endometriosis.Corrects urinary incontinence by supporting and repositioning the bladder.Anesthesia Administration:General Anesthesia: Induces a temporary loss of consciousness, ensuring the patient is unaware and doesn't experience pain during the procedure.Regional Anesthesia: Numbs specific regions of the body, often used for lower abdominal or pelvic surgeries.Surgical Techniques and Instruments Used:Laparoscopic Surgery: Involves small incisions and the use of a camera (laparoscope) to visualize and perform the surgery with specialized instruments.Robotic-Assisted Surgery: Utilizes robotic systems to enhance precision and allow for minimally invasive procedures.Traditional Open Surgery: In certain cases, an open approach may be necessary, involving a larger incision for direct access to the pelvic organs.During the surgery, the surgical team employs these techniques and instruments based on the nature of the procedure and the patient's specific needs. The choice between different surgical approaches often depends on factors like the complexity of the surgery, the patient's health status, and the surgeon's expertise.After the Surgery1. Immediate Recovery in the Hospital:Monitoring: Patients are closely monitored in the initial postoperative period to ensure stability and detect any complications.Vital Signs: Regular checks on vital signs, such as heart rate and blood pressure, are conducted.Pain Management: Intravenous pain medications may be administered as needed.2. Pain Management:Medications: Prescription or over-the-counter pain relievers are provided to manage postoperative discomfort.Patient Communication: Open communication with healthcare providers helps tailor pain management strategies to individual needs.Non-Pharmacological Approaches: Techniques like deep breathing exercises and guided imagery may complement pain medications.3. Physical Activity and RehabilitationGradual Mobilization: Encouraging patients to move gradually helps prevent complications and promotes blood circulation.Physiotherapy: Rehabilitation programs, including physiotherapy, may be recommended to restore strength and flexibility.Activity Restrictions: Certain restrictions on strenuous activities may be advised initially to facilitate proper healing.Latest AdvancementsMinimally Invasive Techniques (laparoscopic, robotic):Advances in technology have led to the widespread adoption of minimally invasive procedures.Smaller incisions, reduced pain, faster recovery, and lower risk of complications are associated with laparoscopic and robotic-assisted surgeries.Eligibility for these techniques depends on factors such as the nature of the surgery and the patient's overall health.Enhanced Recovery After Surgery (ERAS) Protocols:ERAS focuses on optimizing perioperative care to expedite recovery.Includes preoperative education, optimized nutrition, early mobilization, and multimodal pain management.Shorter hospital stays, faster return to normal activities, and improved patient satisfaction are outcomes associated with ERAS.These advancements underscore a shift towards patient-centric care, aiming to enhance recovery experiences and outcomes. Minimally invasive techniques and ERAS protocols reflect a commitment to reducing the physical and emotionalTips for Preparing YourselfUtilize relaxation techniques and meditation.Communicate openly with healthcare providers to address concerns.Seek support from friends and family.Adhere to preoperative dietary guidelines.Stay well-hydrated.Incorporate light, approved exercises.Ask questions about potential risks and expected outcomes.:Be aware of infection, bleeding, and anesthesia-related risks.Ensure strict adherence to sterile techniques during surgery.Risks and ComplicationsThe most common complication of pelvic surgery is infectionInfection:Introduction of bacteria during surgery or postoperative care.Symptoms may include fever, redness, swelling, or discharge at the surgical site.Bleeding:Excessive bleeding during or after surgery.Can lead to complications such as anemia or the need for additional interventions.Adverse Reactions to Anesthesia:Allergic reactions or complications related to the administration of anesthesia.Monitoring vital signs is crucial to identify and address any adverse responses.Strategies to Prevent ComplicationsMaintain a sterile environment in the operating room to minimize the risk of infections.Proper hand hygiene, sterilization of instruments, and aseptic procedures are essential.Thorough Preoperative Assessment:Comprehensive evaluation of the patient's health status before surgery.Identify and manage pre-existing conditions that may increase the risk of complications.:Continuous monitoring of vital signs in the immediate postoperative period.In summary, pelvic surgery is a vital intervention addressing diverse pelvic health issues. Patient preparation is crucial for a successful surgical experience, emphasizing mental readiness, physical well-being, and understanding the procedure. Advances in surgical techniques and postoperative care contribute to improved outcomes, making pelvic surgery a transformative solution for enhanced quality of life.

Minimally Invasive Urological Surgery : Healing with Precision
Minimally Invasive Urological SurgeryWhen we talk about Minimally Invasive Urological Surgery, we're referring to a modern approach that focuses on performing surgical procedures with the least amount of disruption to the body. Unlike traditional open surgeries, these techniques involve small incisions and advanced technology, allowing for precision and reduced impact on the patient.The journey of Minimally Invasive Techniques in urology is quite fascinating. Traditionally, surgeries involved large incisions, longer recovery times, and increased discomfort. However, with advancements in technology, techniques like laparoscopy and robotics have revolutionized how we approach urological procedures. This evolution has paved the way for more patient-friendly interventions.Why does Minimally Invasive Urological Surgery matter? Well, the importance lies in its ability to offer a host of advantages to patients. By opting for smaller incisions and innovative tools, surgeons can perform complex procedures with heightened precision. This not only leads to reduced pain but also translates into shorter hospital stays and quicker recovery times. Beyond the physical benefits, it significantly contributes to an overall improvement in the patient's well-being.Types of Minimally Invasive Urological SurgeryA. Laparoscopic SurgeryBasic Principles : Laparoscopic urological surgery involves the use of a thin, lighted tube (laparoscope) and small incisions through which specialized instruments are inserted. The laparoscope transmits images to a video monitor, guiding the surgeon throughout the procedure. Basic principles include:Pneumoperitoneum: The abdomen is inflated with carbon dioxide to create a working space.Trocar Placement: Ports or trocars are inserted through small incisions for instrument access.Minimally Invasive Access: Smaller incisions result in reduced trauma and quicker recovery.Instruments UsedLaparoscope: Fiber-optic camera for visual guidance.Trocar and Cannulas: Access ports for instruments.Graspers, Scissors, and Dissectors: Specialized tools for manipulating tissues.Electrocautery Devices: Used for cutting and coagulation.Common Laparoscopic Urological ProceduresLaparoscopic Nephrectomy: Removal of the kidney.Laparoscopic Prostatectomy: Treatment for prostate cancer.Laparoscopic Pyeloplasty: Repair of a blocked ureteropelvic junction.B. Robotic-Assisted SurgeryRobotic Technology : Robotic urological surgery involves the use of a surgical robot controlled by the surgeon from a console. The da Vinci Surgical System is a common example. Key components include:Robotic Arms: Mimic the surgeon's hand movements.Console: Where the surgeon sits and controls the robot.3D Imaging: High-definition 3D visualization.Advantages and LimitationsAdvantages:Enhanced precision and dexterity.Reduced surgeon fatigue.3D visualization for better depth perception.Limitations:Cost of equipment and maintenance.Steeper learning curve for surgeons.Robotic Urological ProceduresRobotic Prostatectomy: Removal of the prostate for prostate cancer.Robotic Partial Nephrectomy: Partial removal of the kidney.Robotic Cystectomy: Removal of the bladder.C. Endoscopic SurgeryTechniques and Equipment : Endoscopic urological surgery involves the use of small cameras and instruments inserted through natural body openings or small incisions. Techniques and equipment include:Cystoscopy: Examination of the bladder using a cystoscope.Ureteroscopy: Visualizing the ureter and kidney using a ureteroscope.Transurethral Resection of the Prostate (TURP): Treatment for prostate enlargement.Applications in UrologyStone Removal: Endoscopic procedures for kidney stones.Bladder Tumor Removal: Transurethral resection for bladder tumors.Ureteral Stricture Repair: Endoscopic treatment for ureteral strictures.Common Endoscopic Urological ProceduresFlexible Ureteroscopy: Exploration of the ureter and kidney.Transurethral Bladder Tumor Resection: Removal of bladder tumors.Percutaneous Nephrolithotomy (PCNL): Removal of large kidney stones.In summary, laparoscopic, robotic-assisted, and endoscopic urological surgeries offer diverse approaches, each with its unique set of advantages and applications in the treatment of urological conditions.Surgical TechniquesA. Trocar Placement and Access: Trocar placement involves the insertion of small, tubular instruments through minimal incisions, creating access points for surgical tools. This technique minimizes tissue trauma and facilitates the introduction of specialized instruments.B. Intraoperative Imaging: Intraoperative imaging refers to the use of various imaging modalities during surgery to enhance visualization. This aids surgeons in precisely navigating and conducting procedures with improved accuracy.C. Procedure-specific Techniques:Nephrectomy: Nephrectomy is the surgical removal of a kidney. This procedure can be performed using minimally invasive techniques, involving smaller incisions for reduced postoperative discomfort.Prostatectomy: Prostatectomy is a surgical intervention for prostate cancer. Minimally invasive approaches, such as robotic or laparoscopic prostatectomy, allow for smaller incisions and potentially faster recovery.Pyeloplasty: Pyeloplasty is a reconstructive surgery to correct ureteropelvic junction obstruction. Minimally invasive methods, including laparoscopy, aim to restore normal urine flow with less impact on surrounding tissues.Cystectomy: Cystectomy involves the removal of the bladder, often necessary in cases of bladder cancer. Minimally invasive approaches aim to reduce recovery time and postoperative complications by using smaller incisions.These surgical techniques showcase advancements in urological procedures, emphasizing precision, reduced invasiveness, and improved patient outcomes.What does minimally invasive urological surgery treat?Minimally invasive urological surgery is employed to treat a variety of urological conditions and diseases. Some of the common conditions that can be addressed through minimally invasive techniques include:Prostate Conditions:Prostate Cancer: Minimally invasive approaches, such as robotic-assisted laparoscopic prostatectomy, are frequently used for the surgical removal of the prostate in cases of prostate cancer.Benign Prostatic Hyperplasia (BPH): Conditions causing prostate enlargement, like BPH, can be treated through procedures such as transurethral resection of the prostate (TURP) using endoscopic techniques.Kidney Conditions:Kidney Stones: Flexible ureteroscopy or percutaneous nephrolithotomy (PCNL) can be employed to remove kidney stones through minimally invasive means.Renal Tumors: Nephrectomy (partial or complete removal of the kidney) can be performed using minimally invasive techniques for renal tumors.Bladder Conditions:Bladder Cancer: Cystectomy, the removal of the bladder, may be performed using minimally invasive approaches.Bladder Stones: Endoscopic procedures can be used to remove stones from the bladder.Ureteral Conditions:Ureteral Obstructions: Conditions causing blockages in the ureter, such as ureteropelvic junction (UPJ) obstruction, can be treated with pyeloplasty using minimally invasive techniques.Testicular Conditions:Testicular Cancer: In some cases, minimally invasive techniques may be used for lymph node dissection or other procedures related to testicular cancer.Pelvic Organ Prolapse:Pelvic Organ Prolapse: Procedures to address pelvic organ prolapse, such as sacrocolpopexy, can be performed through minimally invasive means.Incontinence:Urinary Incontinence: Certain minimally invasive procedures, like the placement of slings, can be used to address urinary incontinence.Comparative Analysis with Traditional Open urological SurgeriesAspectMinimally InvasiveTraditional Open SurgeryIncision SizeSmall (<1 inch)Larger, several inchesBlood LossReducedHigher risk of blood lossPain and DiscomfortReduced postoperative painMore significant pain, longer recoveryHospital StayShorterLongerRecovery TimeQuickerSlowerCosmetic ImpactMinimal scarringNoticeable scarringTechnical ComplexitySpecialized training requiredGeneral expertise may sufficeCostHigher initial costsPotentially lower initial costsComplication RatesLowerHigherInfection RiskReducedHigherPatient SatisfactionHigher satisfactionVaried satisfactionBenefits of Minimally Invasive Urological Surgery:Reduced postoperative painFaster recovery timesEnhanced surgical precisionLower infection riskImproved cosmetic outcomesRisks and Considerations:Technical complexity and specialized trainingLearning curve for surgeonsHigher initial equipment costsLimited suitability for all patients or conditionsPossibility of converting to open surgery based on intraoperative findingsEmerging Technologies and Future Directions1. Advancements in Robotics: Robotics is witnessing a transformative evolution with enhanced dexterity in robotic arms. The exploration of remote surgery possibilities and improvements in haptic feedback systems are notable. The integration of artificial intelligence further augments these systems, providing surgeons with greater control and adaptability.2. Innovations in Imaging: The integration of 3D imaging and augmented reality is reshaping the visualization landscape during surgery. Real-time imaging technologies continue to advance, offering continuous guidance for precise navigation. Future directions may involve incorporating functional imaging modalities, and artificial intelligence plays a crucial role in expediting data interpretation.3. Integration of Artificial Intelligence: Artificial intelligence is poised to revolutionize urological surgery. Machine learning algorithms are anticipated to enhance preoperative planning and predict patient outcomes. AI-driven robotic systems are expected to actively participate in real-time decision-making, and the application of AI in data-driven personalized medicine will optimize treatment plans based on individual patient data.Minimally invasive urological surgery (MIS) is a safe and effective treatment option for most urological conditions. MIS offers a number of advantages over traditional open surgery, including less pain, shorter hospital stays, and faster recovery times. MIS is also associated with a reduced risk of complications.MIS is now the standard of care for many urological procedures, and it is likely to play an even greater role in the future.

All about urethroplasty : What you need to know
Urethra is like a tiny tunnel responsible for letting pee out. Now, sometimes things go a bit wonky in that tunnel, and that's where urethroplasty swoops in like a superhero.Urethroplasty is basically the fixer-upper for your urethra. It's a surgical magic trick where doctors repair or reconstruct that little tube, so it works the way it's supposed to.Now, why does this matter? Well, imagine your urethra as a traffic cop for your pee. When it's not working right, things get chaotic. Urethroplasty steps in to restore order. It's like saying, "Hey, let's get this traffic flowing smoothly again!" It's not just about fixing pipes; it's about making your daily life less complicated. So, urethroplasty is a bit of a pee-hero, making sure you can go about your business without any trouble.Indications for UrethroplastyA. Reasons:Urethral Strictures: Narrowing that obstructs urine flow, necessitating corrective intervention.Urethral Injuries: Addressing trauma-induced damage to ensure proper healing and functionality.Hypospadias Repair Complications: Resolving issues arising from previous surgical procedures for hypospadias.Other Urethral Abnormalities: Tackling congenital or acquired variations affecting normal urethral function.B. Candidates:Men with Obstructed Urine Flow: Suitable for those facing obstruction due to urethral strictures, seeking restoration of unimpeded urine flow.Patients with Recurrent Urethral Infections: Addressing chronic infections and complications that may lead to structural damage.Individuals with Congenital Urethral Abnormalities: Tailored intervention for those with birth-related structural issues affecting the urethra.Urethroplasty serves as a personalized approach to restore normalcy in function and structure, ensuring comprehensive care for individuals with diverse urological challenges.Procedure for Urethral SurgeryA. Before Surgery (Preoperative Phase)Patient Evaluation and Preparation: The journey toward healing begins with a thorough assessment of the patient's medical history and physical condition. Careful consideration is given to individual health factors, ensuring the most tailored and effective approach.Imaging Studies: Precision is key. Advanced imaging studies are conducted to provide a comprehensive understanding of the urethral structure. This aids the surgical team in planning a meticulous intervention.Discussion of Potential Risks and Benefits: Patient engagement is a cornerstone. Open dialogue ensues, enlightening the patient on the intricacies of the procedure, potential outcomes, and associated risks. A well-informed patient is a partner in the healing process.B. During Surgery (Intraoperative Phase)Anesthesia Administration: Comfort and safety intertwine as anesthesia is administered, ensuring a pain-free and secure environment for the surgery to unfold.Incision and Exposure of the Urethra: With utmost precision, a skilled surgical team delicately exposes the affected area. Every incision is made with care, marking the beginning of the therapeutic journey.Excision or Repair of the Affected Segment: Surgical finesse comes into play as the damaged segment is either excised or meticulously repaired. Every action is guided by the commitment to restore optimal function and well-being.Tissue Grafting or Substitution: Innovative techniques are employed, such as tissue grafting or substitution, to ensure the seamless reconstruction of the urethra. The goal is not just repair but restoration to a state of health and vitality.C. After Surgery (Postoperative Phase)Catheterization: A critical aspect of recovery, catheterization is performed with precision to facilitate healing. This essential step promotes optimal urinary function during the initial stages of recovery.Wound Care and Monitoring: Each wound is a testament to the body's resilience. Diligent care is administered, and continuous monitoring ensures any signs of healing or complications are promptly addressed.Pain Management: Compassion meets expertise in the management of postoperative pain. Tailored approaches ensure that discomfort is minimized, allowing the patient to focus on their recovery journey.Follow-up Appointments for Evaluation: The healing process is a collaborative effort. Scheduled follow-up appointments are integral, allowing the medical team to assess progress, address any concerns, and guide the patient towards complete recovery.In every phase, from the initial evaluation to the postoperative follow-up, the procedure is not just a medical intervention but a holistic approach to restoring health and well-being. The journey is navigated with precision, compassion, and a commitment to the patient's optimal outcome.Latest Advancements in Urethroplasty:Tissue Engineering:Creating functional tissue constructs to enhance natural healing.Benefits: Reducing complications associated with traditional grafts.Minimally Invasive Techniques:Endoscopic and laser-assisted techniques for less invasive procedures.Benefits: Shorter recovery times, reduced pain, and minimized scarring.Robotic-Assisted Urethroplasty:Robotic technology for enhanced precision and control.Benefits: Improved outcomes through precise maneuvers.3D Printing in Urethral Reconstruction:Customized grafts and anatomical models created with 3D printing.Benefits: Personalized surgery for better functional outcomes.Bioabsorbable Stents:Temporary stents that gradually dissolve post-reconstruction.Benefits: Reducing complications associated with long-term stent use.Platelet-Rich Plasma (PRP) Therapy:Using concentrated platelets for enhanced tissue healing.Benefits: Adjunct therapy to improve success rates and speed up healing.Always consult with healthcare professionals for the latest information, as advancements may vary by facility and case.Preparation Tips for PatientsGet a clear picture of what's ahead to make informed decisions about your upcoming procedure.Stick to healthcare guidelines, including diet and medications, and complete necessary tests promptly for a smooth process.Openly communicate with your healthcare team, seeking clarification on the procedure, risks, and what to expect afterward.Proactively prepare your mind and emotions. Explore relaxation techniques to manage anxiety and foster a positive outlook.Risks and ComplicationsInfection: Potential for postoperative infections, requiring vigilant monitoring and prompt intervention.Bleeding: Risk of bleeding during or after the procedure, necessitating careful management.Urethral Stricture Recurrence: Possibility of the urethral stricture reoccurring, requiring additional intervention.Erectile Dysfunction (in Some Cases): In certain instances, a risk of erectile dysfunction may be associated with the procedure.Strategies to Prevent ComplicationsAntibiotic ProphylaxisAdministering prophylactic antibiotics before surgery to reduce the risk of infection.Strict Adherence to Postoperative CareEnsuring meticulous adherence to postoperative care instructions for optimal recovery.Regular Follow-up AppointmentsScheduling and attending regular follow-up appointments to monitor progress and address any emerging issues promptly.In a nutshell, urethroplasty isn't just a fix—it's a significant improvement for those dealing with urethral challenges. Whether it's a narrow passage, injuries, or quirks, this procedure restores comfort and normalcy. The key? Open communication with your healthcare team.
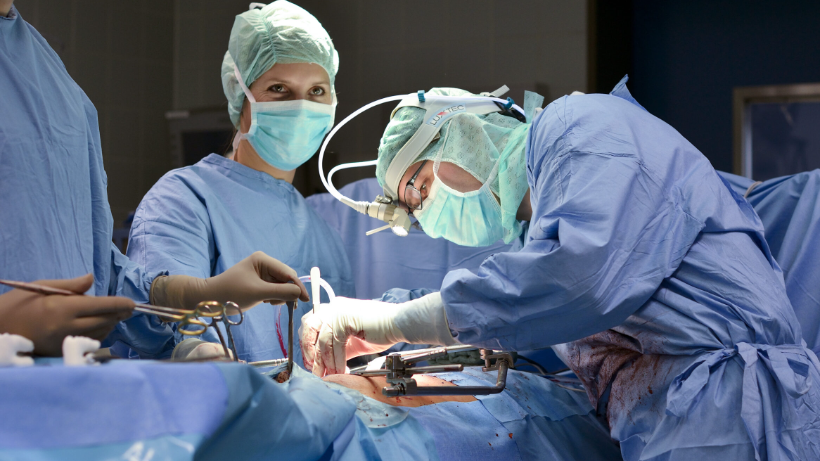
Know everything about Prostate Cancer surgery (Prostatectomy)
This blog serves as a guide through the intricacies of prostate cancer surgery, from understanding the basics to navigating the postoperative landscape. Join us as we explore the significance of surgery in treating prostate cancer, the latest innovations shaping the field, and practical tips for patients preparing for this critical step in their healthcare journey.Prostate cancerProstate cancer is a type of cancer that develops in the prostate, a small walnut-shaped gland in men that produces seminal fluid. This cancer usually grows slowly and remains confined to the prostate gland initially, but in some cases, it can be aggressive and spread to other parts of the body.Role of Surgery in Prostate Cancer TreatmentSurgery is one of the primary treatment options for prostate cancer, aiming to remove the cancerous tissue and potentially cure the disease. The two main types of surgical procedures for prostate cancer are radical prostatectomy and robotic-assisted laparoscopic prostatectomy. The choice of surgery depends on factors such as the stage of cancer, the patient's overall health, and the surgeon's expertise.Why Prostate Cancer Surgery is PerformedCurative Intent: The primary goal of prostate cancer surgery is to remove the cancerous prostate gland and surrounding tissues to eliminate or control the cancer.Localized Cancer: Surgery is particularly effective when the cancer is confined to the prostate and has not spread beyond its boundaries.Prevention of Spread: Removing the cancerous prostate can prevent the spread of cancer to other organs and tissues.Who Benefit from SurgeryLocalized Cancer: Surgery is most beneficial for patients with early-stage prostate cancer that is localized to the prostate gland.Long Life Expectancy: Patients with a longer life expectancy and good overall health are often considered suitable candidates for surgery.Aggressive Tumors: In cases where the cancer is more aggressive, surgery may be recommended to remove the tumor before it has a chance to spread.Younger Patients: Younger patients may opt for surgery as it offers the potential for a cure and long-term cancer control.Adverse Pathological Features: Patients with adverse pathological features, such as high-grade tumors or involvement of the prostate margins, may benefit from surgery to remove as much cancerous tissue as possible.Types of Prostate Cancer SurgeryA. Radical ProstatectomyOpen Surgery- This is like the traditional way. A surgeon makes a large incision to access the prostate. It's like opening a big book to get to the page you want.Laparoscopic Surgery - Here, smaller incisions are made, and a tiny camera helps the surgeon see inside. It's like prostate surgery with mini tools!. Think of it as a keyhole surgery adventure.Robot assisted surgery- Picture a surgeon controlling a robot with super-precise moves. It's like playing a video game with life-saving consequences. A high-tech surgery buddy – the surgeon guides a robot to do the delicate work.B. Transurethral Resection of the Prostate (TURP)TURP is a bit different. No external cuts here. Instead, a tool goes in through the urethra to remove part of the prostate causing trouble. It's like fixing a clogged pipe from the inside.So, to sum it up, we've got the classic 'Open Surgery,' the cool 'Laparoscopic' adventure, and the futuristic 'Robotic-Assisted' teamwork. And then there's 'TURP,' a bit like internal plumbing magic. Different strokes for different folks, or in this case, different surgeries for different situations!Preoperative Phase: Getting Ready for Prostate Cancer SurgeryA. Diagnostic Tests and AssessmentsThink of it as the detective work before the action movie. Doctors need to know the enemy (cancer) and the battlefield (your body).Tests: Blood tests, imaging (like MRI or CT scans), and sometimes a biopsy.B. Patient PreparationPhysical and Mental Preparationit's like gearing up for a marathon. Exercise, good food – getting your body in the best shape.It's also a mind game. Understanding the process, talking to loved ones – mental strength is crucial.Medication AdjustmentsSome meds might need to take a back seat temporarily. The doctors don't want any unexpected plot twists during surgery.Your superhero team (doctors) will guide you on what meds to pause and what to keep.C. Informed ConsentIt's like signing up for a mission. Before the surgery adventure begins, you need to know the risks, benefits, and alternatives.Your surgeon will explain everything – the what, why, and how of the surgery. Ask questions – it's your script too!D. Preoperative InstructionsIt includes when to stop eating (you don't want a full stomach on the surgical roller coaster) and when to arrive.Pack your essentials – ID, insurance info, and comfy clothes for post-surgery.this phase as the calm before the storm – getting everything ready for the big show. Tests and prep ensure everyone's on the same page, physically and mentally. It's like gearing up for a superhero mission – you need the right tools, the right mindset, and a clear plan. Intraoperative Phase: Inside the Prostate Cancer Surgery TheaterA. Operating Room Setup This like setting up the stage for a play. The room is clean, tools are sterilized, and everyone has their role.Surgeons, nurses, and maybe even the superhero robot – everyone's in place.B. Anesthesia AdministrationIt's the 'lights out' moment before the show begins. Anesthesia ensures you're comfortable and asleep during the surgery.General anesthesia (like deep sleep) or sometimes regional anesthesia (just the lower part of your body is asleep).C. Surgical Procedure StepsIncision and AccessThe surgeon makes the first move, creating an entrance to the prostate. This could be a classic cut (open surgery), tiny cuts (laparoscopic), or a robot's delicate touch.Removal of Prostate TissueThe focus is on removing the cancerous part of the prostate. The surgeon is like a sculptor, carefully shaping the prostate landscape.Lymph Node Dissection (if required)If the cancer plot threatens to spread, the surgeon might check nearby lymph nodes. It's a preventive measure.D. Robotic-Assisted Surgery AdvancementsIf it's a robotic-assisted surgery, imagine a surgeon guiding a robot with precision. It's like having a high-tech sidekick ensuring accuracy and less invasion.the operating room as the theater, the surgeons as the actors, and anesthesia as the director, ensuring you're in a peaceful sleep. The main plot unfolds as the surgeon delicately removes the cancerous part. If it's a robotic show, it's a tech-savvy superhero duo. Each step is like a scene, bringing us closer to a cancer-free ending.Postoperative Phase: After the Prostate Cancer Surgery Curtain FallsA. Recovery Room CareNurses monitor you closely, ensuring a smooth transition from the surgical stage to waking reality.Think of it as the cast and crew making sure everything's okay post-show.B. Hospital Stay DurationThe duration depends on the type of surgery and how well you're recovering. It's like staying in a hotel where your health is the VIP guest.C. Catheterization and Urinary Function A catheter might be your post-surgery companion. It helps drain urine while your body adjusts.You'll get instructions on catheter care and tips for when it's finally removed.D. Pain ManagementPost-Show Discomfort: It's normal to feel some discomfort after the surgical spotlight. Pain meds are the backstage crew making sure you're comfortable.Communication is Key: Let your healthcare team know about your pain level – they'll adjust the script accordingly.E. Early Ambulation and RehabilitationGetting Back in the Groove: Early movement is like the first steps after intermission. It prevents complications and gets you back on your feet.Guided Steps: Physiotherapy might be in the script to ensure a smooth return to normal activities.F. Potential ComplicationsUnexpected Plot Twists: Complications are the plot twists no one wants. They could be bleeding, infection, or issues with urinary function.Superhero Response: Your healthcare team is ready for anything. Early detection and treatment are their superhero moves.The postoperative phase is like the aftermath of a grand performance. You move from the recovery room to a sort of health hotel, with catheters, pain management, and guided steps back to normalcy. And like any good story, there might be unexpected twists, but your superhero healthcare team is there to ensure a happy ending. Latest Advancements in Prostate Cancer SurgeryA. Robotic Surgery InnovationsIntroduction of Surgical Sidekick: Imagine a surgeon with a high-tech sidekick – that's robotic surgery. It's not just a tool; it's a precision assistant.Precision Personified: Robotic arms with tiny instruments allow for extremely precise movements, reducing invasiveness and speeding up recovery.B. Minimally Invasive TechniquesSmall Cuts, Big Impact: Surgeons are now opting for smaller incisions, like keyholes, for certain procedures.Faster Recovery: Less cutting means quicker healing. It's like a streamlined version of traditional surgery.C. Targeted TherapiesBullseye on Cancer: It's not just about removing the bad part; it's about hitting it with precision. Targeted therapies focus on specific molecules involved in cancer growth.Personalized Medicine: Treatment that's tailored to your unique cancer profile, aiming for maximum effectiveness with minimal side effects.Tips for Patient PreparationA. Mental and Emotional Preparation:Understand the Procedure:Educate yourself about the surgery and what to expect.Attend informational sessions or ask your healthcare team questions.Emotional Well-being:Seek emotional support from family, friends, or support groups.Consider counseling or therapy if needed.B. Physical Conditioning:Regular Exercise:Engage in light exercises like walking or stretching to improve overall fitness.Consult with your healthcare team for exercise recommendations.Healthy Diet:Maintain a balanced diet rich in nutrients to support recovery.Follow any dietary guidelines provided by your healthcare team.C. Communication with Healthcare Team:Open and Honest Communication:Clearly communicate your concerns, expectations, and any pre-existing conditions.Discuss medications, allergies, and follow preoperative instructions carefully.Questions and Clarifications:Don't hesitate to ask questions about the procedure, potential side effects, and postoperative care.Ensure you fully understand the information provided.D. Support System Establishment:Identify Supportive Individuals:Build a support network of family and friends who can assist during recovery.Communicate your needs and expectations with your support systemCaregiver Preparation:Provide information to caregivers about your surgery and recovery plan.Ensure they are aware of postoperative responsibilities and potential challenges.How can we help with the treatment?If you're on the lookout for treatment in India, let Healthtrip be your compass. We will serve as your guide throughout your medical treatment. We'll be by your side, in person, even before your medical journey commences. The following will be provided to you:Connect with renowned doctors from a network spanning 35+ countries and access the world's largest health travel platform.Collaboration with 335+ top hospitals , including Fortis and Medanta.Comprehensive treatments from Neuro to Cardiac to Transplants, Aesthetics, and Wellness.Post-treatment care and assistance.Teleconsultations at $1/minute with leading surgeons.Trusted by 44,000+ patients for appointments, travel, visa, and forex assistance.Access top treatments and packages, such as Angiograms and many more.Gain insights from genuine patient experiences and testimonials.Stay updated with our medical blog.24/7 unwavering support, from hospital formalities to travel arrangements or emergencies.Pre-scheduled specialist appointments.Prompt emergency assistance, ensuring safety.Our patient success stories See more inspiring testimonials of HealthtripRisks and Complications of Prostate Cancer SurgeryProstate cancer surgery, while often effective, comes with potential risks and complications. It's crucial to be aware of these factors as they can impact the overall treatment experience. Here's a breakdown:Infection:Risk: Surgical procedures create openings that may introduce infections.Prevention: Strict adherence to preoperative hygiene protocols and prescribed antibiotics.Bleeding:Risk: Surgical procedures involve cutting, which can lead to bleeding.Prevention: Precise surgical techniques and temporary cessation of blood-thinning medications.Erectile Dysfunction:Risk: Surgery may impact nerves and blood vessels essential for erections.Prevention: Discussion with the surgical team about potential effects and consideration of nerve-sparing techniques.Incontinence:Risk: Disruption of urinary control mechanisms during surgery.Prevention: Pelvic floor exercises (Kegels) before and after surgery, and gradual resumption of normal activities.Outlook and Follow-up CareA. Expected Recovery Timeline:Gradual Progress:Understand that recovery is a step-by-step process, and improvements may take time.Realistic expectations for returning to normal activities.B. Follow-up Appointments:Regular Check-ins:Attend scheduled follow-up appointments as recommended by your healthcare team.Discuss any concerns or changes in your health during these visits.C. Monitoring PSA Levels:Periodic Tests:Regular monitoring of Prostate-Specific Antigen (PSA) levels to track cancer recurrence.PSA tests are part of ongoing surveillance for any signs of prostate cancer activity.D. Lifestyle Modifications for Long-Term Health:Healthy Habits:Adopting a balanced diet with emphasis on fruits, vegetables, and whole grains.Regular exercise and maintaining a healthy weight for overall well-being.Prostate cancer surgery, or prostatectomy, is a key treatment for localized cases. It offers tailored approaches, including robotic techniques, with ongoing advancements improving outcomes. In summary, it's a crucial intervention in the fight against prostate cancer.






